cara mengobati penyakit herpes agar tidak kambuh lagi - banyak para penderita penyakit herpes menginginkan kesembuhan yang cepat tanpa memikirkan apakah pengobatan yang dilakukan aman dan tanpa efek samping dan apakah Obat Penyakit Herpes Ampuh merupakan pengobatan yang dilakukan mampu mengobati penyakit herpes dengan tuntas ? Banyak para penderita penyakit herpes yang mengeluh karena di kemudian hari penyakit yang di derita kambuh lagi. Lalu bagaimana pengobatan yang tepat untuk penyakit herpes?
Obat Penyakit Herpes Ampuh – Herpes dapat masuk menginfeksikanya melalui hubungan baik secara mulut dan seks, herpes merupakan sebuah penyakit yang dapat menular melalui hubungan seks ciri khas herpes ialah ada lepuhan pada area mulut kelamin biasanya berupa benjolan berisi oleh air yang akan pecah dengan sendirinya. Penyakit Herpes kelamin adalah penyakit yang disebabkan oleh virus Herpes kelamin 1 (HSV-1) dan virus Herpes kelamin 2 (HSV-2). Infeksi kedua jenis herpes virus ini berbeda satu sama lain melihat tempat infeksi HSV 1 dan HSV 2 berbeda.
PENYAKIT HERPES
Herpes merupakan salah satu jenis penyakit yang sangat mudah sekali untuk menular, jadi hati-hati dan jaga kontak fisik dengan penderita herpes. Herpes itu sendiri juga di bedakan menjadi beberapa macam, sesuai dengan penyebabnya yaitu herpes simplek yang ditandai dengan luka seperti melepuh dan berisi air, herpes zoster merupakan jenis herpes yang terjadi karena penyakit varisella yang kambuh lagi, herpes genital yang berada di daerah alat kelamin, herpes labialis jika herpes terdapat pada bibir.
Herpes merupakan jenis penyakit yang disebabkan oleh virus, maka dari itu antibiotik seperti amoxcilin, ampicillin dan sodara-sodaranya nggak akan mempan untuk meredakan herpes. Karena herpes merupakan penyakit yang di akibatkan oleh virus, obatnya pun yang harus untuk membunuh viru bukan antibiotik yang berguna untuk membunuh bakteri. Ada beberapa tips yang bia kita lakukan sebagai cara mengobati herpes. Seperti apa caranya, kita lihat yuk
Herpes merupakan salah satu jenis penyakit yang sangat mudah sekali untuk menular, jadi hati-hati dan jaga kontak fisik dengan penderita herpes. Herpes itu sendiri juga di bedakan menjadi beberapa macam, sesuai dengan penyebabnya yaitu herpes simplek yang ditandai dengan luka seperti melepuh dan berisi air, herpes zoster merupakan jenis herpes yang terjadi karena penyakit varisella yang kambuh lagi, herpes genital yang berada di daerah alat kelamin, herpes labialis jika herpes terdapat pada bibir.
CIRI DAN GEJALA PENYAKIT HERPES
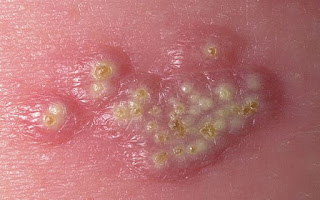
Ciri-ciri penyakit herpes yang mudah dikenali adalah timbulnya bulatan-bulatan kecil berisi cairan bening. Cairan ini bila pecah dan dibiarkan sampai kering akan terlihat seperti koreng. Karena penyakit herpes merupakan penyakit yang mudah menular, maka sebaiknya segera diobati sebelum menyebar lebih parah.
Penyakit herpes merupakan penyakit yang meradang pada kulit dan biasanya muncul gelembung yang berisi air dan berkelompok. Penyakit Herpes terdiri dari dua macam yaitu herpes zoster, penyakit herpes yang menyerang kulit. Dan herpes genitalis adalah penyakit herpes yang merupakan salah satu penyakit kelamin. Ciri-ciri herpes ini yaitu rasa sesak nafas, demam, mengigil, sendi terasa nyari, pegal hanya pada satu bagian tubuh saja.
cara mengobati penyakit herpes Biasanya ciri-ciri penyakit herpes lainya yang menyerang penderita penyakit herpes kadang merasa dirinya terserang usus buntu, migraine atau serangan jantung. Kemudian akan muncul gelembung kecil di daerah punggung tetapi pada 1 sisi saja yaitu pada daerah persarafan tertentu. Gelembung tersebut terasa nyeri dan bisa pecah sehingga dapat terinfeksi oleh bakteri.
Herpes kelamin yang sudah mengjangkiti seseorang akan ditandai dengan adanya kesemutan, rasa tidak nyaman atau rasa gatal yang dirasakan beberapa jam sampai 2-3 hari sebelum timbulnya lepuhan. Lepuhan yang dikelilingi oleh daerah kemerahan dapat muncul dimana saja pada kulit atau selaput lendir, tetapi paling sering ditemukan di dalam dan disekitar mulut, bibir dan alat kelamin. Lepuhan (yang bisa saja terasa nyeri) cenderung membentuk kelompok, yang bergabung satu sama lain membentuk sebuah kumpulan yang lebih besar.
Selain itu gejala Herpes kelamin lainnya bisa berupa lecet atau borok (paling sering terdapat di bibir mulut, gusi, dan alat kelamin), pembesaran kelenjar getah bening di leher atau selangkangan (biasanya hanya pada saat infeksi awal), demam lepuh (terutama pada episode pertama), lesi genital (mungkin akan ada sensasi terbakar atau kesemutan) dan lain-lain.
BAGAIMAN CARA MENGOBATI PENYAKIT HERPES ITU SENDIRI…???
Untuk Sobat yang sedang mencari pengobatan penyakit herpes De Nature Menyediakan obat herbal khusus untuk herpes. Penyakit herpes saat ini bisa disembuhkan melalui metode pengobatan tradisional. Seperti yang dilakukan oleh kami.
CV. DE NATURE INDONESIA
De Nature Indonesia adalah sebuah perusahaan yang bergerak di bidang Obat Tradisional (OT)dari dalam Negeri, yang mencoba mengangkat dan menghidupkan kembali Budaya Nenek Moyang kita Yaitu Jamu Tradisional sebagai salah satu warisan leluhur budaya bangsa yang perlu dilestarikan.
Sekedar informasi untuk kenyamanan Konsumen, bahwa Produk dari perusahaan kami ini sudah memiliki:
- Ijin Resmi Perusahaan dari Kementrian Kesehatan
- Ijin BPOM, yang artinya sudah lulus uji stabilitas Produk
- Sertifikat Halal MUI, sehingga kehalalannya bisa dipertanggungjawabkan
- Apoteker Yang berpengalaman
- Sudah melewati Proses Sortir Bahan Baku, Guna Menjaga Mutu Produk
- Proses Produksi Sesuai Alur CPOTB (Cara Pembuatan Obat Tradisional Yang Baik Dan Benar)
Sumber :